 Joshua Zeichner, MD, is the director of cosmetic and clinical research in dermatology at Mount Sinai Hospital in New York City. 
Adalja, MD, is a senior scholar at the Johns Hopkins Center for Health Security. Ramprasad Gopalan, MD, is a Florida-based infectious disease physician.Įudene Harry, MD, is an emergency medicine physician in Orlando, Florida.Īmesh A. Yes, COVID and the flu are two different things, but there will most likely be an increase in the spread of respiratory droplets from people around you sneezing and coughing. (Get vaccinated against COVID-19, get your boosters, and wear a mask when you’re indoors in public areas where the spread of COVID-19 is moderate or severe.) But these steps become even more of a necessity as winter approaches and flu season starts to pick up. You can still take certain measures to protect yourself, of course. Sign up for WH+ for unlimited site access and more There is still plenty of research to be done on these cases, but in the meantime, taking expert advice is crucial. Meanwhile, others are struggling with the side effects of long COVID and are constantly looking for answers as to why their symptoms haven't cleared up. You may even have your own at-home COVID-19 test in your medicine cabinet for the just in case. By now, you've probably become somewhat of an expert on how to keep you and those around you safe, as well as the main symptoms and what to do if you develop them (quarantine ASAP). Then in late November 2021, Omicron made its way to the states for yet another wave of the pandemic.Īlthough restaurants are back in service, kids are back in school, the corporate world is slowly but surely recovering, and cases are down, people are still being diagnosed with COVID everyday. And, unfortunately, new cases still continue to occasionally spike across the country.īy early 2021, the Delta variant caused nearly 99 percent of COVID-19 cases in the country. has now been living with COVID-19 for more than two years. And make sure to isolate if you are sick.įor information on how to find health care, visit our COVID-19 resources page.The U.S. If you are experiencing any of the above symptoms, call your doctor for advice. Symptoms vary based on age and underlying health conditions, but those listed above are the most common. We still have a lot to learn when it comes to COVID-19. Scientists hope to have more concrete findings in the future. 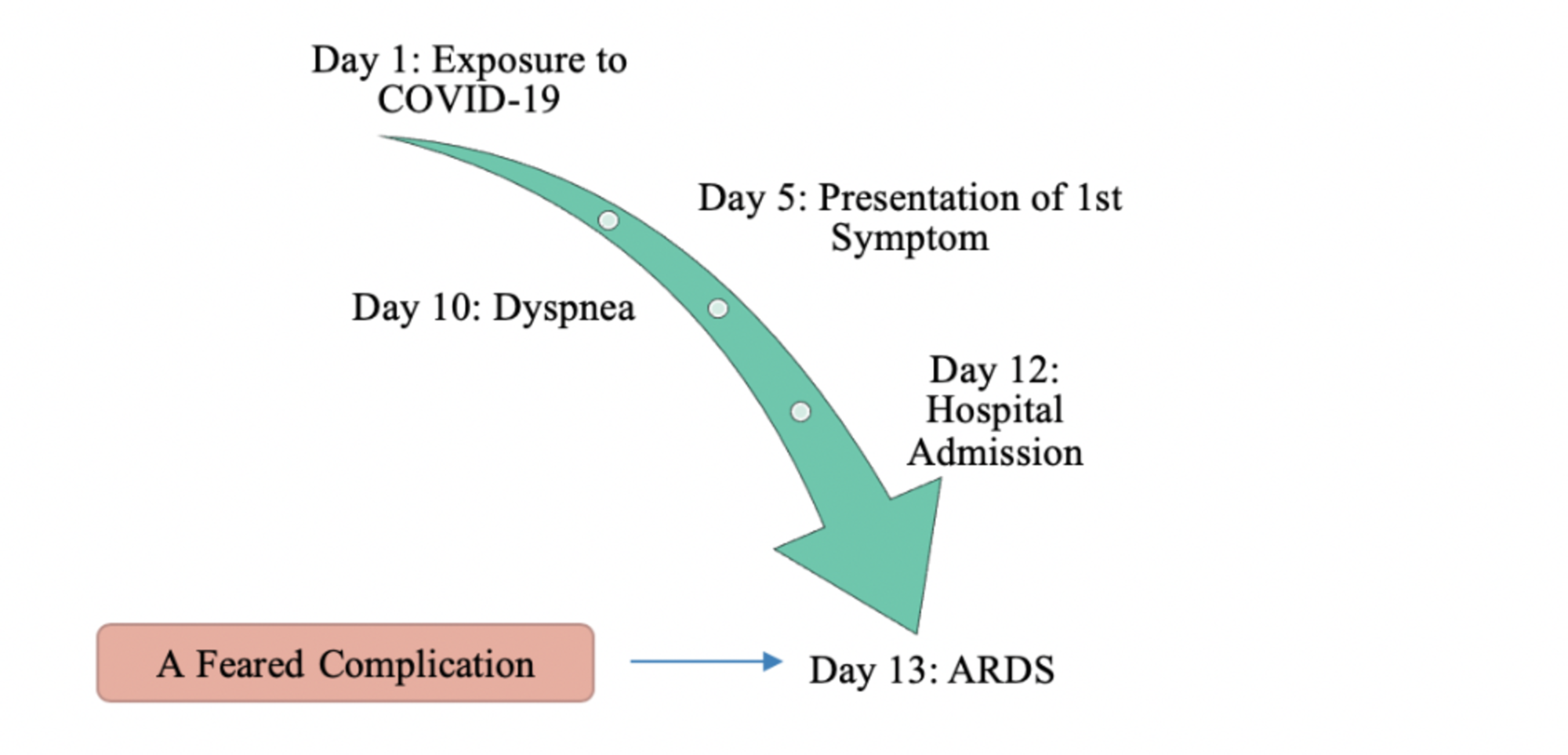
Researchers will continue to study these cases. Some may run the risk of losing it permanently due to the body attacking the nasal passage when fighting COVID-19. For those with severe COVID-19 cases, some have reported losing their sense of smell for months. Typically, when the virus passes and swelling goes down, your sense of smell come back. This is when the tissue around the part of your nose responsible for smell swells up. Initial research about prolonged loss of smell says that patients typically lose their sense of smell because of cleft syndrome. Researchers are still trying to identify why some people experience symptoms for longer than other. These complications may occur as late as three weeks after onset of the initial illness. Bacterial infection is one possible complication. These include fever, loss of taste or smell, fatigue and a prolonged cough.ĬOVID-19 can damage the heart and kidneys. While most symptoms will disappear on their own, some people have reported specific symptoms lingering. Prolonged Recovery and other complications Follow the directions of your provider, contact tracer or other public health provider. This is typically done no sooner than 14 days after diagnosis. Any cough will last an average of 19 days.ĭoctors recommend that people get re-tested to make sure they no longer test positive for the disease. 
If someone has a mild case of COVID-19, this is typically when they begin to feel better. Onset of difficulty breathing may be sudden. But sometimes it occurs as late as 15 days after beginning of any symptoms. The CDC does note that an ARDS diagnosis typically happens between days 8 and twelve. If someone has a severe case of COVID-19, this is typically when they are admitted to the ICU due to acute respiratory distress syndrome (ARDS), extreme difficulty breathing requiring a ventilator.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
